Check my Brain (Black gives way to Blue)
On
The stats are pretty awful. AD and the neurodegenerative diseases in general (the most common being Alzheimer’s, Parkinsonism and Motor Neurone Disease) are all increasing in frequency. Neurodegenerative deaths in the over-65 age group have increased 300% in men, and 500% in women since 1995 (1). The standard position is that this increase is due to the fact that we are all living longer, but I do not believe this. Life expectancy has been falling in the USA for the last 3 years (2), and more recently it has begun to fall in the UK also (3). I predict it will soon start falling also in Germany, Ireland, Belgium and Finland.
I’m pretty confident about this prediction because these are the countries that, after the USA and the UK, consume the greatest amounts of processed and ultra-processed foods. Such foods provide plenty of empty calories but little if any nutrients, a toxic combination that leaves the body fat, diabetic and inflamed –the ideal conditions for creating neurodegenerative disease (4). This in my view is a more likely explanation for the increasing number of victims than simple demographics, and it is supported by evidence that Western (processed) diets are more likely to produce neuro-degenerative disease than the nutrient-dense and anti-inflammatory Mediterranean diet (5, 6).
Dale Bredeson, a professor at UCLA and head of LA’s Buck Institute, has already shown that some cases of early onset AD can be reversed with a well-designed broad spectrum nutritional program (7). His work also indicates that there may be many roads to Alzheimer’s, involving different insults such as chronic inflammation, dysnutrition, endocrine changes and exposure to toxins. Dale is an excellent speaker so if you hear that he is coming to lecture at a facility near you, I urge you to go and listen to him.
New research shows that we may be able to achieve even better protection, by targeting not only the body’s general biochemistry but also by regulating the functions of immune cells in the brain. But in order to explain this, we have to take a detour via beta amyloid, diabetes and yeast. Bear (don’t bare) with me …
A build-up of beta amyloid in the brain has long been recognised as a hallmark of Alzheimer’s, and a number of pharma approaches to beta amyloid reduction have been tried – with null results. One problem is that beta amyloid is not a static target; the amyloid in the plaques is dynamic, ie there are processes that form it and other processes that remove it. It is only when the rates of deposition outstrip the rates of removal that the amyloid plaque grows, and starts to kill significant numbers of neurones.
In the diabetic, beta amyloid formation and deposition is increased. But so is chronic inflammatory stress, and there are also disruptions in various cell signalling pathways; so there are many ways in which diabetes creates a tendency to lose your mind. To put this in context, an out-of-control food industry has now left almost half of all adult Americans with metabolic syndrome or Type 2 diabetes (8). From this perspective, the current figures for dementia and early neurodegenerative death have nowhere to go but up.
Taking more exercise and eating less sugars and starches (the cure for Type 2 diabetes) is, therefore, a legitimate preventative strategy. However, for an even more protective approach, we can also work on the amyloid removal side of the equation. To achieve this, we must focus on the brain’s immune system.
The immune cells in the brain are mostly microglia, and these have many roles in brain function. Some of them are good, and some are not so good. On the plus side microglia do their best to kill off pathogens, should any manage to enter the brain. On the minus side they can, if over-activated, cause inflammation which can make brain disease worse. But it is their third main action that may be the most relevant here. They remove beta amyloid.
The microglia have, on the surface of their cell membranes, a receptor called TREM2. TREM2 recognises beta amyloid, and binds to it; and this binding instructs the microglia to go after the beta amyloid and break it down (9).
Mutations in this receptor which make the microglial cell less able to bind to beta amyloid are associated with rapidly worsening Alzheimers. Conversely, adding TREM2 to knock-out mice bred without TREM2, stops the otherwise inevitably rapid progression of the disease (10).
The above research was led by Professor Huaxi Xu, director of the Neuroscience Initiative at the Sanford Burnham Prebys Medical Research Institute in La Jolla. He struck a note of caution. “It could be beneficial in early stages to activate microglia to eat up amyloid beta’, Xu stated, ‘but if you over-activate them, they may release an overabundance of cytokines and cause extensive inflammation. This would damage healthy nerves and synapses in the vicinity.’
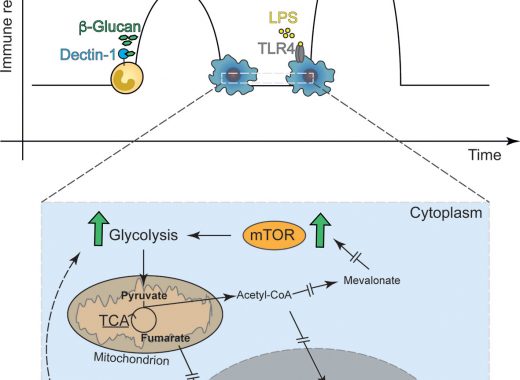
And this is where old-fashioned bakers yeast comes in. Bakers yeast (aka Saccharomyces cerevisiae) contains compounds called 1-3, 1-6 beta glucans, and these stimulate the microglia very effectively indeed – without triggering excess cytokine release (11). And they do one other, very interesting thing. In an unrelated study, the beta glucans were found to increase the regenerative capacity of brain cells (12); to such an extent that they enabled severed optic nerves to heal. The evidence suggests that the ability of the brain to repair damage is mediated via the immune system, and our sterile times – characterized by a lack of beta glucan – not only makes us more allergic (see previous posts), but also prevents the brain from healing after injury.
The above suggests that the amended hygiene hypothesis, which links yeast exposure to allergy, may need to be extended to cover Alzheimers as well.
But could a pinch of bakers yeast really provide protection against Alzheimers, and improve brain resilience in general?
When I introduced the 1-3, 1-4 beta glucans at a UK nutritional science conference in 1996, I was roundly (and publically) criticized by a very established Professor for suggesting that a humble household item could increase resistance to infection. In his defence, he was unaware of the several hundred papers in the literature which showed that the beta glucans did just that; and just because I was right then does not make me right now. But from what I have seen, I think that adding a pinch of the 1-3, 1-6 beta glucans to your daily regime could prove to be an excellent investment in your long-term health.
References:
- JAMA 2017, and https://www.cdc.gov/features/alzheimers-disease-deaths/index.html
- CDC National Center for Health Statistics: https://www.bloomberg.com/news/articles/2018-09-19/five-things-you-need-to-know-to-start-your-day
- Hiam L, Harrison D, McKee M, Dorling D. Why is life expectancy in England and Wales ‘stalling’? J Epidemiol Community Health. 2018 May;72(5):404-408.
- Bharadwaj P, Wijesekara N, Liyanapathirana M, Newsholme P, Ittner L, Fraser P, Verdile G. The Link between Type 2 Diabetes and Neurodegeneration: Roles for Amyloid-β, Amylin, and Tau Proteins. J Alzheimers Dis. 2017;59(2):421-432.
- Romagnolo DF, Selmin OI. Mediterranean Diet and Prevention of Chronic Diseases. Nutr Today. 2017 Sep; 52(5): 208–222.
- Gardener H, Caunca MR. Mediterranean Diet in Preventing Neurodegenerative Diseases. Curr Nutr Rep. 2018 Mar;7(1):10-20.
- Bredesen DE. Reversal of cognitive decline: a novel therapeutic program. Aging (Albany NY). 2014 Sep;6(9):707-17.
- https://www.cdc.gov/diabetes/pdfs/data/statistics/national-diabetes-statistics-report.pdf
- Zhong L, Wang Z, Wang D, Wang Z, Martens YA, Wu L, Xu Y, Wang K, Li J, Huang R, Can D, Xu H, Bu G, Chen XF. Amyloid-beta modulates microglial responses by binding to the triggering receptor expressed on myeloid cells 2 (TREM2). Mol Neurodegener. 2018 Mar 27;13(1):15.
- Zhao Y, Wu X, Li X, Jiang LL, Gui X, Liu Y, Sun Y, Zhu B, Piña-Crespo JC, Zhang M, Zhang N, Chen X, Bu G, An Z, Huang TY, Xu H. TREM2 Is a Receptor for β-Amyloid that Mediates Microglial Function. Neuron. 2018 Mar 7;97(5):1023-1031.e7.
- Shah VB, Huang Y, Keshwara R, Ozment-Skelton T, Williams DL, Keshvara L. Beta-glucan activates microglia without inducing cytokine production in Dectin-1-dependent manner. J Immunol. 2008 Mar 1;180(5):2777-85.
- Baldwin KT, Carbajal KS, Segal BM. Neuroinflammation triggered by β-glucan/dectin-1 signaling enables CNS axonregeneration. Proc Natl Acad Sci U S A. 2015 Feb 24;112(8):2581-6.